Why does mucus build up in the airways of patients with cystic fibrosis?
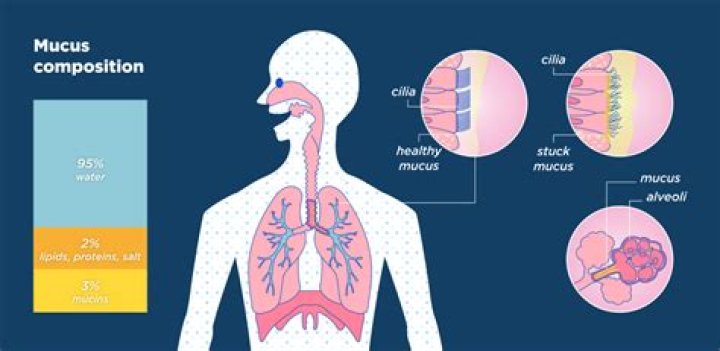
CF causes thick mucus to build up and clog certain parts of the body such as the lung. The buildup is caused by an abnormal gene called CFTR (cystic fibrosis transmembrane regulator). CFTR controls the flow of water and salt in and out of the body’s cells. Changes cause mucus to become thickened and sticky.
What is the mucus like that is in the lungs when a person has cystic fibrosis?
In cystic fibrosis, the airways fill with thick, sticky mucus, making it difficult to breathe. The thick mucus is also an ideal breeding ground for bacteria and fungi. Cystic fibrosis (CF) is an inherited disorder that causes severe damage to the lungs, digestive system and other organs in the body.
How does cystic fibrosis affect ventilation?
How does CF affect the respiratory system? The abnormal electrolyte transport system in CF causes the cells in the respiratory system, especially the lungs, to absorb too much sodium and water. This causes the normal thin secretions in the lungs to become very thick and hard to move.
Where does mucus build up in cystic fibrosis?
What is cystic fibrosis (CF)? Cystic fibrosis (CF) is a genetic (inherited) disease that causes sticky, thick mucus to build up in organs, including your lungs and pancreas. If you don’t have CF, the mucus that lines organs and body cavities, such as your lungs and nose, is slippery and watery.
How does mucus affect breathing?
In response to the inflammation, excess mucus is produced. This can block the small airways and reduce respiratory efficiency, for example, in chronic airways obstruction. Over-production of mucus leads to frequent coughing, which further irritates the tissues and causes even more mucus production.
What color is cystic fibrosis mucus?
Really dark brown, tenacious phlegm is seen in patients who have cystic fibrosis or bronchiectasis, which is a chronic lung disease. The phlegm is brown because of blood and the intense chronic inflammation that comes with the chronic disease state.
Does cystic fibrosis affect gas exchange?
In patients with cystic fibrosis (CF) the architecture of the developing lungs and the ventilation of lung units are progressively affected, influencing intrapulmonary gas mixing and gas exchange.
How is the digestive system affected by extra mucus in CF?
About 90 percent of people with CF have sticky mucus that blocks ducts in the pancreas and prevents enzymes from reaching the small intestine to digest food. Undigested food in the intestines can cause pain, cramping, gas and either loose, greasy, floating stools or constipation and blockages.
What is mucus made of?
Mucus is a slippery, gelatinous goo produced by your mucous membranes. It lines your mouth, nose, throat, sinuses, lungs, and gastrointestinal tract. It’s made up of 95% water, with a mix of glycoproteins, proteoglycans, lipids, proteins, and DNA.
What is the mechanism of mucus accumulation in cystic fibrosis (CF)?
Mucins, the high-molecular-weight glycoproteins responsible for the viscoelastic properties of the mucus, play a key role in the disease but the actual mechanism of mucus accumulation is still undetermined. Multiple hypotheses regarding the impact of CFTR malfunction on mucus have been proposed and are reviewed here.
What is the pathophysiology of CFCF?
CF is caused by mutations in the cystic fibrosis transmembrane conductance regulator (CFTR) gene and is characterized by the accumulation of thick, adherent mucus plaques in multiple organs, of which the lungs, gastrointestinal tract and pancreatic ducts are the most commonly affected.
What is cystic fibrosis (CF)?
Cystic fibrosis (CF) is both the most common and most lethal genetic disease in the Caucasian population.
Where are mucins secreted in the lungs?
In the lungs, gel-forming mucins are secreted by goblet cells distributed throughout the conducting airways and submucosal glands located in the large airways. 4, 5 Airway goblet cells secrete MUC5B and MUC5AC to produce a thin mucus layer that lines the epithelial surfaces.